 The events of the previous year shed a much needed light on disparities in our healthcare system. Recently, we sat down with Loral Patchen, PhD, CNM, and IBCLC at MedStar Washington Hospital Center, to discuss her experiences using technology to serve diverse populations and impact healthcare justice.
The events of the previous year shed a much needed light on disparities in our healthcare system. Recently, we sat down with Loral Patchen, PhD, CNM, and IBCLC at MedStar Washington Hospital Center, to discuss her experiences using technology to serve diverse populations and impact healthcare justice.
Dr. Patchen is a midwife, but also a scientist, researcher, and program director driving innovation at MedStar Washington Hospital Center, and brings a uniquely diverse experience to the question.
At first pass, her advocacy for technology might seem unusual for a midwife. Far from depersonalizing the care experience, Dr. Patchen believes that technology can be used to enhance high touch care; and foster community, group-based care, and connect patients to their social workers.
We’ve pulled out some of her most important points from the webinar.
[Listen to the full recording]
On Structural Inequity
“We’ve been dealing with unique times and circumstances this year, starting with the particular incidences of police brutality against Black Americans. These questions have achieved more attention recently, but they are ever-present and they shape the context in which we deliver care.
We have to consider population health differently than individual health. What we experience as individuals is different than what a population experiences, and we have to consider this in the medical field. Race may be a socially-constructed variable, but we have to pay attention to it.
Black women do not experience poor maternal outcomes as a group because of their biology but because of failures in the system.
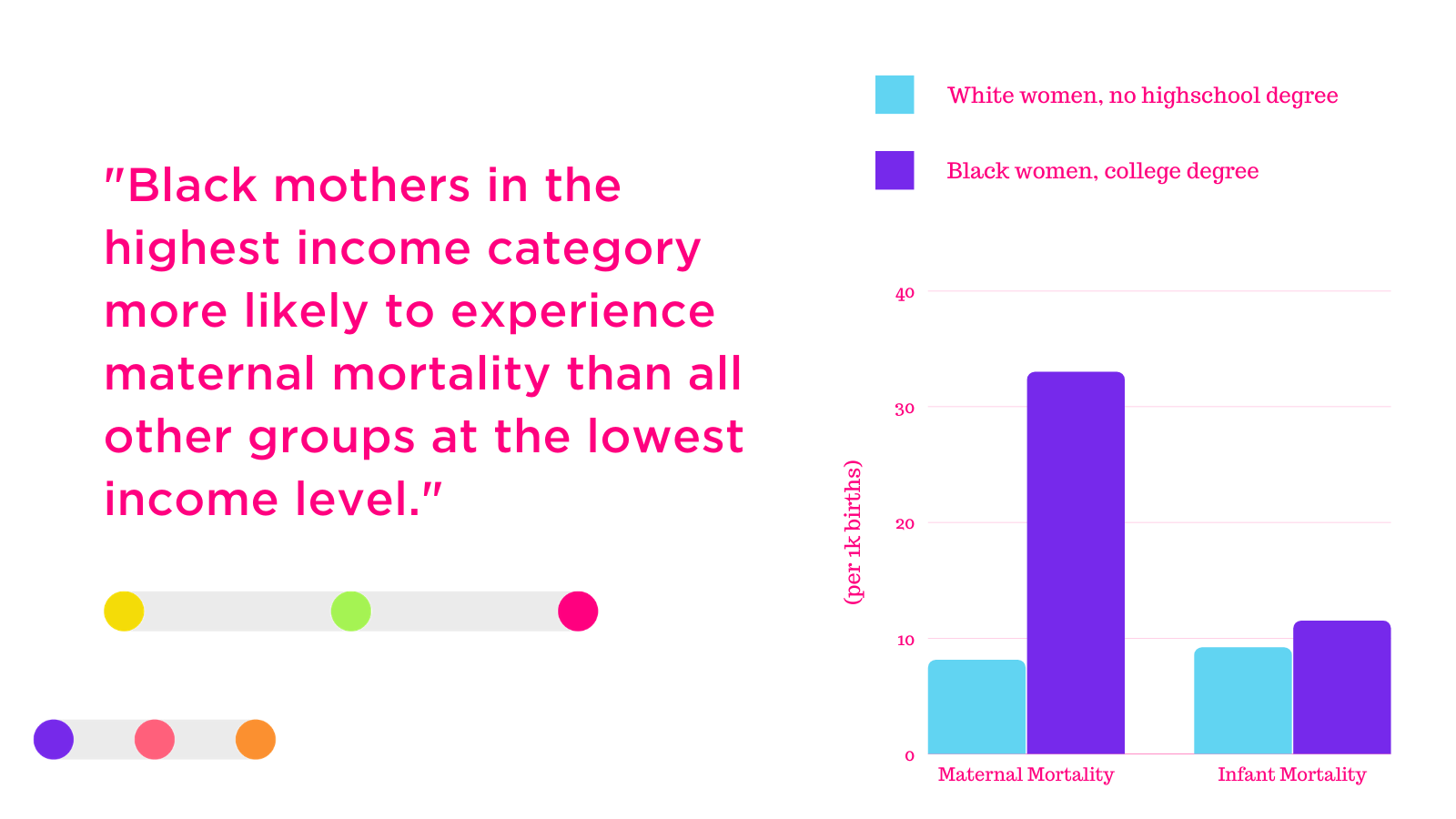
Take two case studies as an example: Lisa is a white, non-highschool graduate. She works 20/hrs a week at a grocery store for minimum wage, and is getting her GED. She is expecting a baby girl in December.
Mary is a Black graduate of Howard. She has a law degree, and earns 250k a year. She is also expecting a baby girl in December.
Of these two pregnant women, Mary is more likely to have a catastrophic outcome in childbirth and/or have her infant die in the first year after birth.
On the Role of the Provider in Combating Inequity
The opportunity to improve the system lies in community and social contexts and in the healthcare system — as providers we have a particular opportunity for impact because of our interaction with patients.
Consequences of structural inequities that we encounter:
- Suspicion
- Fear
- Fewer health care visits
- Early termination of treatment
- Delayed seeking of care
- Mistrust
We cannot directly control these things as providers, but they’re profoundly connected to our patients' experience of the healthcare system, and we do need to navigate these things even if we cannot directly control them.
The pathway towards this comes through improving health literacy, trust, greater patient agency vs. improved pharma, advancements in surgical tech, more screenings, and perhaps most importantly, cultivating a sense of patient ownership in their own health outcomes and creating a safe space from this.”
On the Role of Babyscripts in Combating Inequity
I believe that technology helps providers deliver on these objectives, and our experience with Babyscripts at MedStar has borne this out.
Babyscripts helps improve health literacy through
- Customizable content (meeting rapidly evolving patient expectations)
- Selection of visuals
- Language to reflect the populations that we serve
- Intentional selections to counteract harmful narratives
Having control over this content helped us to truly hone in on positive narratives, like celebrating black motherhood. The reading level at our health system is widely variable and diverse (people with Phds, people who are illiterate), so it is equally important to have visuals and content for low literacy and higher literacy. Our patient populations demand sophistication: content that includes both.
Health literacy helps provide a level playing field. Women rely a lot on their smartphones for maternal health information. When we are the ones that provide the info, it takes them out of the position of having to search for themselves and gives them a resource bank to do more research for themselves.
Babyscripts helps us promote a connection to our specific practice. We have practice-specific info, pictures of the team, contact info, etc., which helps build and foster connection. We deliver real time info to patients, which has never been more important than in the last year in response to Covid. We could reassure patients that they were getting access to the most up-to-date info as soon as it was available, and also keep them updated on anything new and unique to our practice.
The more that you customize, the more patients engage. It’s not something extra, but something connected to the choice that they made and the community of providers that they trust.
On Provider Benefits
With ready access to high quality, scientifically accurate content, patients can read about their stage or symptoms in advance of their appointment, which frees up more time in the encounter to focus on the patient’s priorities and needs.
This access to information between visits has reduced and improved triage — patients have the right contact info, and the calls that we get are the calls we really need to get. Patients are accessing and using the system more consistently in the ways that we hope.
On Blood Pressure Monitoring
Remote blood pressure monitoring through Babyscripts promotes patient agency and cements the connection between the individual and their own health data.
Blood pressure became a very real and routine focal point in an appointment after high-profile Black mothers Beyonce and Serena Williams shared their experiences with preeclampsia. Our minority patients especially were asking questions about how to monitor their own blood pressure and what we would do to monitor it.
Blood pressure monitoring increases the awareness of its importance, and putting the agency in the hands of the patient helps us move forward in terms of resolving inequities. Getting the patient invested during the onboarding process is an essential part of this success — if a patient feels that the provider is trying to have less contact or offload the burden of care onto their shoulders, they will be turned off. These tools have to be presented as tools of empowerment, that will increase convenience and deliver safer care.
On Reimbursement
There are great philanthropic opportunities for delivering technology to underserved populations, but also opportunities for reimbursement. Babyscripts is a sustainable option for us because there are codes that reimburse and it does not require outside support.
Key Takeaways
Using Babyscripts,
- Improves access to information
- Improves alignment of info in regard to the patient
- Places more agency in the hands of the patient
- Offers more data, more quickly, to providers to improve clinical decisions
- Breaks down elements of system intimidation
- Minimizes exposures to elements of the system that harm black women, until we achieve more substantive changes in delivery of care
Listen to the full recording for more insights, including two case studies involving high blood pressure readings and interventions, and tune in to Dr. Patchen’s question and answer session addressing topics like reimbursement, delivery of blood pressure cuffs, and other best practices.

Submit a comment